Vascular Surgery
Vascular Surgery Department
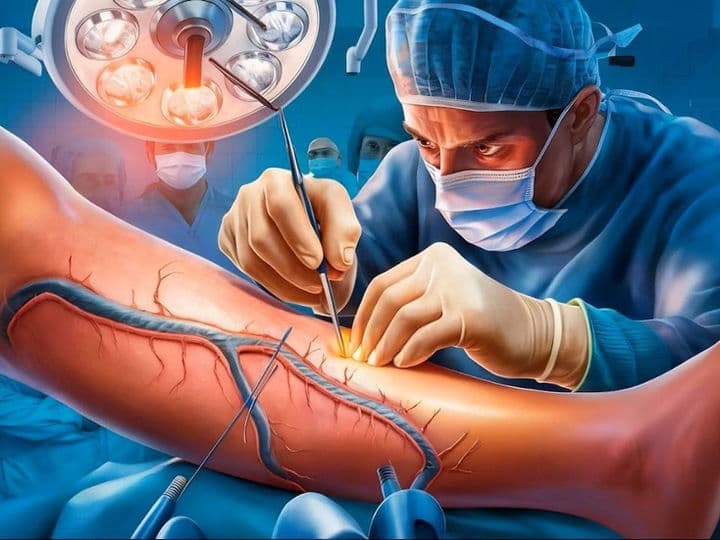
The Vascular Surgery Department is the hospital’s specialized "circulation hub," dedicated to the vast and intricate network of arteries and veins. While cardiac surgeons focus on the heart, vascular surgeons manage every blood vessel from the neck to the toes. For international patients, this wing represents the pinnacle of modern "plumbing" science, utilizing both traditional open surgery and high-tech "endovascular" interventions to ensure every organ and limb receives the life-sustaining blood flow it requires.
A Specialized Team of Circulation Experts
Vascular care is a multidisciplinary field where surgical mastery meets interventional medicine:
Vascular & Endovascular Surgeons: Primary experts trained in both traditional "open" vessel repair and "keyhole" stent placements.
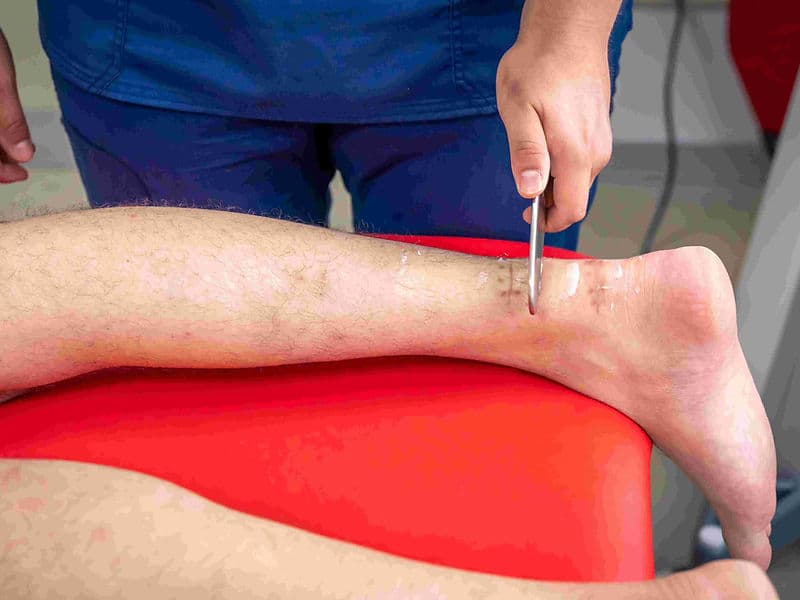
Podiatrists (Limb Salvage Specialists): Experts focused on diabetic foot care and the healing of ulcers caused by poor circulation.
Vascular Technologists: Specialized sonographers who use Doppler ultrasound to map blockages, clots, and leaky valves in real-time.
Wound Care Specialists: Clinical nurses expert in treating chronic sores and skin changes resulting from venous insufficiency.
Advanced Infrastructure and Endovascular Technology
The department utilizes high-resolution imaging and miniaturized hardware to restore blood flow with minimal trauma:
The Hybrid Cath Lab: A futuristic surgical suite that allows for minimally invasive stent procedures with the capability to switch to open surgery instantly if needed.
Stent-Graft Technology: Fabric-covered mesh "sleeves" used to reinforce aneurysms (vessel bulges) from the inside, preventing life-threatening ruptures.
High-Pressure Angioplasty & Atherectomy: Precision tools that use balloons or rotating "shaving" devices to clear plaque and hard calcium from clogged arteries.
Laser & Radiofrequency Fibers: Modern "incisionless" tools that seal diseased varicose veins from the inside, redirecting blood to healthier pathways.
Vena Cava Filters: Microscopic metal "umbrellas" designed to catch traveling blood clots before they can reach the lungs.
Specialized Functional and Diagnostic Units
To ensure a total recovery, the department houses several dedicated diagnostic and treatment hubs:
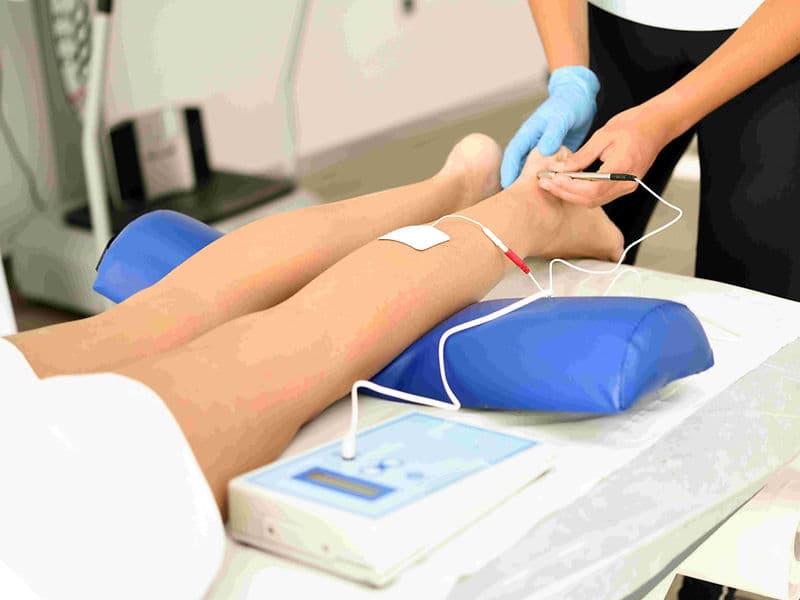
Non-Invasive Vascular Lab: A screening center using the Ankle-Brachial Index (ABI) to compare blood pressure and identify hidden blockages.
The Dialysis Access Clinic: A specialized unit where surgeons create vital "fistulas" for patients requiring long-term kidney dialysis.
Varicose Vein & Daycare Suite: A specialized area for walk-in, walk-out laser treatments for bulging or painful leg veins.
Limb Salvage Center: A high-intensity wing focused on preventing amputations through aggressive circulation restoration in patients with severe peripheral artery disease (PAD).
A Focus on Preservation and Stroke Prevention
The department’s philosophy centers on restoring natural function and preventing emergency events:
Limb Preservation Excellence: Advanced re-opening techniques that have reduced the need for major amputations by over 50% in recent years.
Aneurysm Protection: Repairing aortic bulges through tiny groin punctures rather than large abdominal incisions, significantly lowering patient risk.
Carotid Artery Management: Precision "cleaning" of the neck arteries to significantly reduce the risk of major strokes in high-risk patients.
Emergency Clot Retrieval: Utilizing the legendary Fogarty Catheter to manually retrieve fresh blood clots, saving limbs within the critical "golden hour."
International Patient Support: A dedicated lounge for global families to coordinate 3D CT Angiograms, surgical bookings, and long-term travel plans.