Upper Endoscopy & Colonoscopy
Upper Endoscopy and Colonoscopy
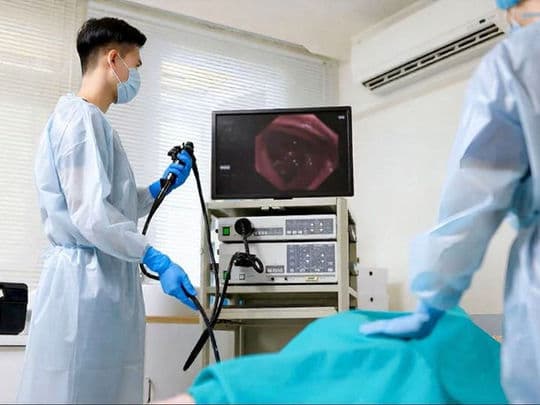
Upper Endoscopy and Colonoscopy are the primary diagnostic tools used to visualize and treat disorders of the digestive tract. While both utilize a high-definition camera at the tip of a flexible tube (an endoscope), they target different regions of the gastrointestinal system and serve distinct medical purposes. Beyond mere visualization, these procedures allow for immediate interventions, such as taking biopsies, treating ulcers, and removing precancerous polyps, often preventing the need for more invasive surgery.
When You Should Consider These Procedures
Upper Endoscopy (EGD): Advised for persistent heartburn (GERD), difficulty swallowing, unexplained upper abdominal pain, or chronic nausea.
Colonoscopy: Recommended for routine colorectal cancer screening (standard starting age is 45), investigating rectal bleeding, or chronic changes in bowel habits.
Anemia Investigation: When blood tests suggest internal bleeding that could be coming from either the upper or lower GI tract.
IBD Monitoring: To assess the health of the intestinal lining in patients with Crohn’s disease or Ulcerative Colitis.
Unexplained Weight Loss: To rule out malabsorption issues (like Celiac disease) or internal malignancies.
Follow-up Care: To monitor the healing of previously diagnosed ulcers or the recurrence of polyps.
Conditions That Require Specialized Care
Barrett’s Esophagus: Requiring high-resolution EGD to monitor for precancerous changes in the esophagus.
Large Polyps: Cases requiring specialized "Endoscopic Mucosal Resection" (EMR) to remove growths without surgery.
Strictures: Narrowing of the esophagus or colon that may require "Dilation" (stretching) during the procedure.
Active GI Bleeding: Emergency cases where the endoscope is used to clip or cauterize a bleeding vessel.
Celiac Disease: Requiring precise biopsies of the duodenum to confirm a diagnosis.
How These Procedures Are Performed
Upper Endoscopy (EGD): A thin, flexible tube is passed through the mouth into the esophagus, stomach, and duodenum while the patient is under light to moderate sedation.
Colonoscopy: The scope is inserted through the rectum to examine the entire length of the large intestine (colon).
AI-Assisted Detection: Modern screenings often utilize artificial intelligence software that highlights flat or small polyps in real-time on the monitor.
Biopsy and Polypectomy: If an abnormality is found, specialized tools are passed through the scope to take tissue samples or remove polyps entirely.
Insufflation: Air or carbon dioxide is used to gently expand the tract, providing a clear and detailed view of the mucosal lining.
Duration: An EGD typically takes 10–15 minutes, while a colonoscopy takes 30–45 minutes.
Innovations in Endoscopy
AI-Enhanced Polyp DetectionSophisticated algorithms that act as a "second set of eyes," helping physicians spot precancerous lesions with significantly higher accuracy.
Disposable High-Definition ScopesThe use of single-use, high-resolution endoscopes in specific cases to eliminate any risk of cross-contamination.
Carbon Dioxide (CO2) InsufflationReplacing room air with CO2, which is absorbed by the body much faster, significantly reducing post-procedure bloating and gas.
Pill-Cam (Capsule Endoscopy)A swallowable camera used to visualize the "middle" part of the small intestine that traditional scopes cannot reach.
Water-Exchange ColonoscopyA technique using water instead of air to navigate the colon, which can lead to a more comfortable experience and higher polyp detection rates.
Advanced Hemostatic ClipsNext-generation tools used during the procedure to instantly stop internal bleeding or close small tears in the intestinal wall.
Pre-Procedure Preparation
EGD Preparation: Requires strict fasting (NPO) for 6 to 8 hours to ensure the stomach is completely empty.
Colonoscopy Preparation: Involves a "clear liquid diet" the day before and the consumption of a laxative solution to clear the colon.
Medication Review: Discussion with the doctor regarding blood thinners or diabetes medications that may need adjustment.
Transportation: Because both procedures involve sedation, patients must arrange for a driver to take them home.
Hydration: Maintaining fluid intake during the prep phase (for colonoscopy) to prevent electrolyte imbalances.
Diagnostic Measurements and Tests
Urease Test (CLOtest): Performed during an EGD to check for H. pylori bacteria, a common cause of ulcers.
Histopathology: Detailed lab analysis of biopsies taken during the procedure to check for cancer or inflammation.
Adenoma Detection Rate (ADR): A quality metric used to ensure the physician is performing a thorough screening.
Terminal Ileum Evaluation: Checking the very end of the small intestine during a colonoscopy to look for signs of Crohn's disease.
Retroflexion: A maneuver where the scope is turned 180 degrees to view the "blind spots" behind folds in the colon or stomach.
Why These Procedures Are Highly Effective
Cancer Prevention: Colonoscopy is one of the few screenings that can actually prevent cancer by removing polyps before they turn malignant.
Immediate Intervention: Diagnosis and treatment (like stopping a bleed or removing a growth) often happen in the same session.
High Accuracy: Provides a direct, high-definition view of the tissue that X-rays or CT scans cannot match.
Minimally Invasive: Offers a way to treat many GI issues without the need for traditional incisions or long hospital stays.
Peace of Mind: Provides definitive answers to chronic symptoms, allowing for targeted and effective medical therapy.
Recovery and Monitoring
Patients move to a recovery area for 1–2 hours until the effects of the sedation wear off.
Minor "gas pain" or bloating is common after a colonoscopy; walking helps the body expel the air used during the test.
A mild sore throat may occur after an EGD; this typically resolves within 24 hours.
Most patients can resume a normal diet immediately, unless specific instructions are given following a large polyp removal.
Results from visual findings are usually shared immediately, while biopsy results may take a few days.
Life After Endoscopy and Colonoscopy
Clearer insight into digestive health and a definitive plan for managing symptoms like acid reflux or IBD.
Protection against colorectal cancer for several years, depending on the findings and the patient's risk profile.
Successful removal of symptomatic polyps or the successful treatment of gastric ulcers.
Enhanced quality of life through the management of chronic GI conditions.
Empowerment to make dietary or lifestyle changes based on the direct visual evidence of the digestive tract’s health.