Ophthalmology
Ophthalmology Department (Eye Care)
The Ophthalmology Department is a globally recognized center of excellence where advanced microsurgery meets the pinnacle of diagnostic science. Because the human eye is a delicate organ only 24mm wide, our department utilizes miniaturized technology to treat it with sub-micron precision. For international patients, we offer a specialized "Center for Sight" that focuses on preserving and restoring the complex biological camera that connects you to the world.
A Multidisciplinary Circle of Vision Experts
Our team is strategically divided into sub-specialties to manage every delicate layer of the eye:
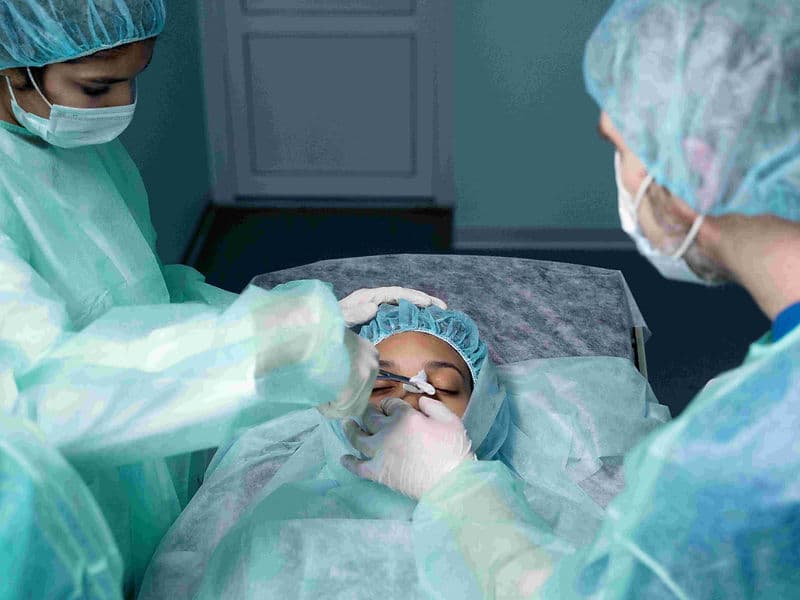
Primary Ophthalmologists: Expert surgeons who lead "blade-free" vision correction and advanced cataract procedures.
Vitreoretinal Specialists: Highly trained surgeons focusing on the back of the eye, treating retinal detachments and diabetic complications.
Cornea & Refractive Experts: Dedicated to the clear front window of the eye, managing corneal transplants and LASIK.
Glaucoma Specialists: Focused on preserving the optic nerve through advanced pressure-management technologies.
Paediatric Ophthalmologists: Providing gentle, specialized care for children's vision, including squint and lazy eye correction.
Ocularists & Optometrists: Professionals dedicated to custom prosthetic fitting and comprehensive visual acuity mapping.
Advanced Technology for Precision Care
To ensure the safest outcomes, the department utilizes world-class laser systems and high-power magnification:
"Blade-Free" Laser Systems: Utilizing Excimer and Femtosecond lasers to reshape the cornea with accuracy impossible for the human hand.
Phacoemulsification (Phaco): Advanced ultrasonic technology that dissolves cataracts through a tiny 2mm opening for stitch-free healing.
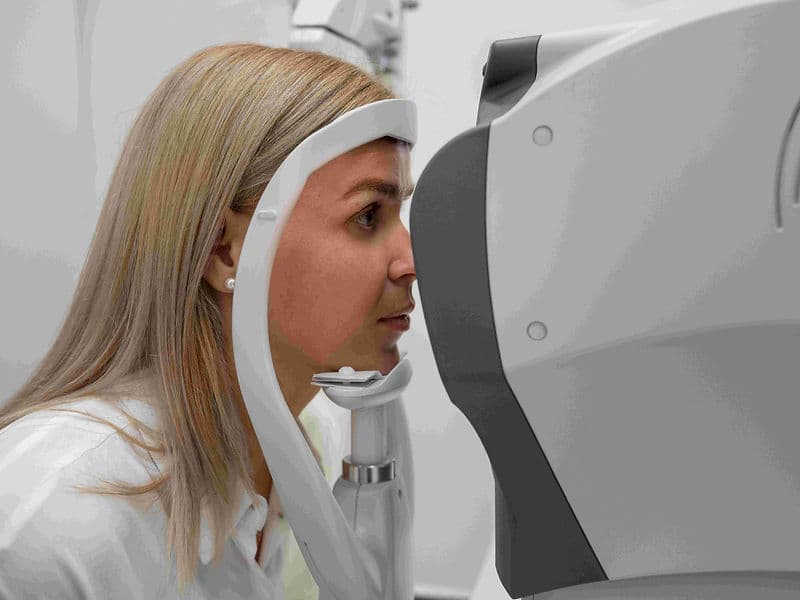
OCT (Optical Coherence Tomography): An "ultrasound with light" that provides high-resolution 3D cross-sections of the retina to catch issues early.
Next-Gen Intraocular Lenses (IOLs): Premium, foldable lenses that replace the eye’s natural lens to restore clear, multifocal vision.
Digital Fundus Mapping: High-speed wide-angle cameras that create a permanent "map" of your retina for long-term monitoring.
Specialized Functional and Diagnostic Units
Our department functions as a self-contained hub for all vision-related needs:
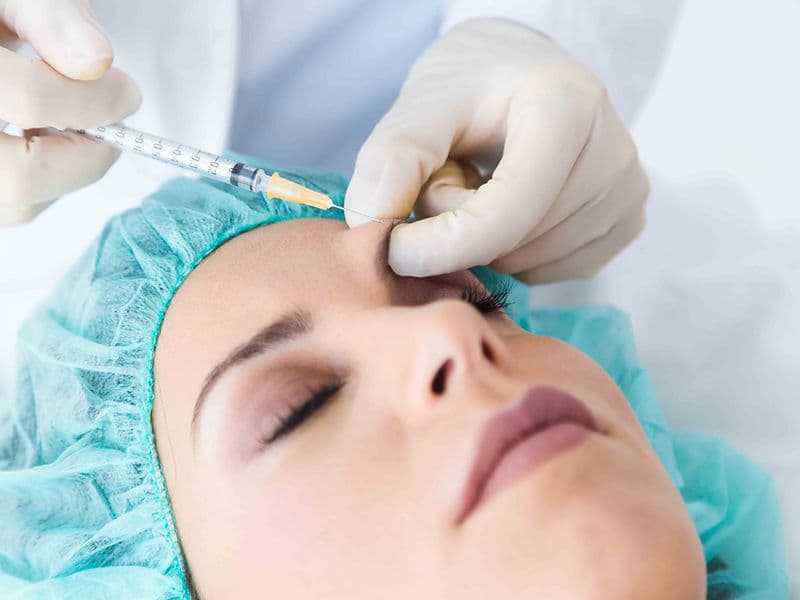
The Sterile Injection Suite: A dedicated environment for administering advanced therapies for macular degeneration and retinal swelling.
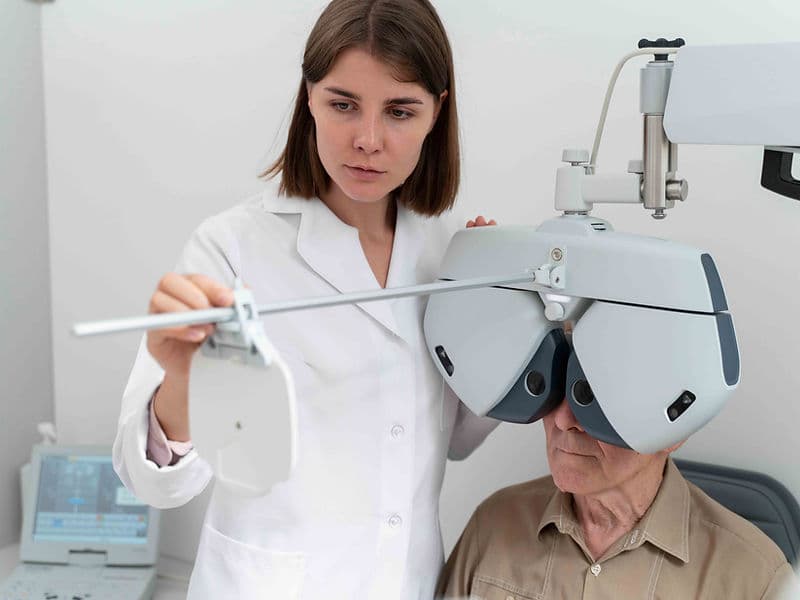
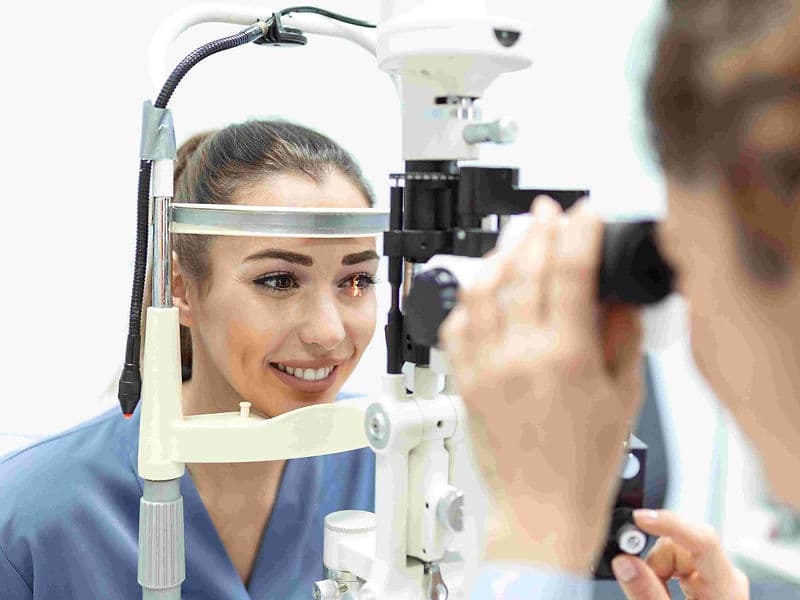
Advanced Refraction Rooms: Specialized dark rooms designed for precise mapping of visual acuity and prescriptions.
High-Tech Laser Wing: Housing YAG and Argon lasers for non-invasive treatments of cloudy capsules and diabetic eye disease.
Contact Lens & Scleral Clinic: A dedicated station for fitting specialized lenses for irregular corneal conditions like Keratoconus.
International Patient Support Lounge: A private space for global families to manage insurance, medical records, and travel logistics in comfort.
A Commitment to Rapid Recovery and Visual Clarity
The modern patient journey is designed for safety, comfort, and immediate results:
Micro-Incisional Surgery: Most procedures are "stitch-free," allowing natural healing and a return to daily activities within days.
No-Stitch Cataract Solutions: Modern IOLs can correct for both distance and reading, often providing the best vision of a patient's life.
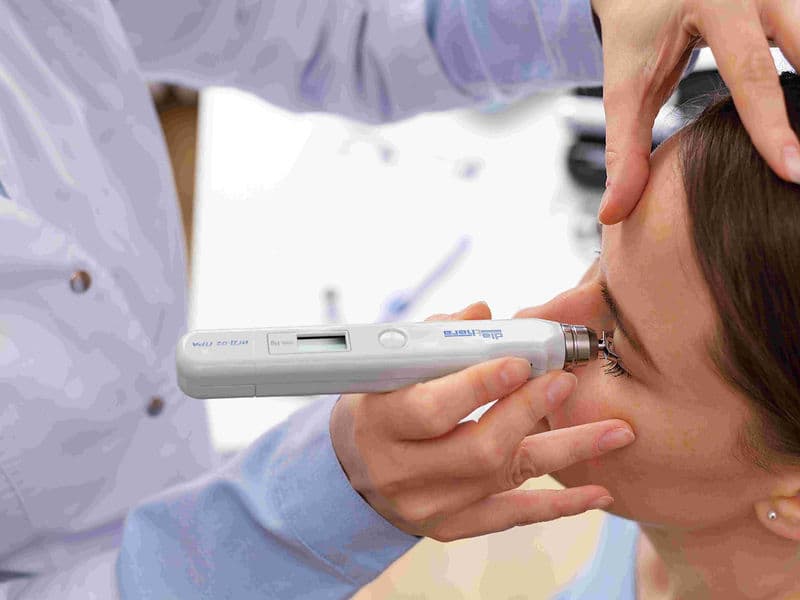
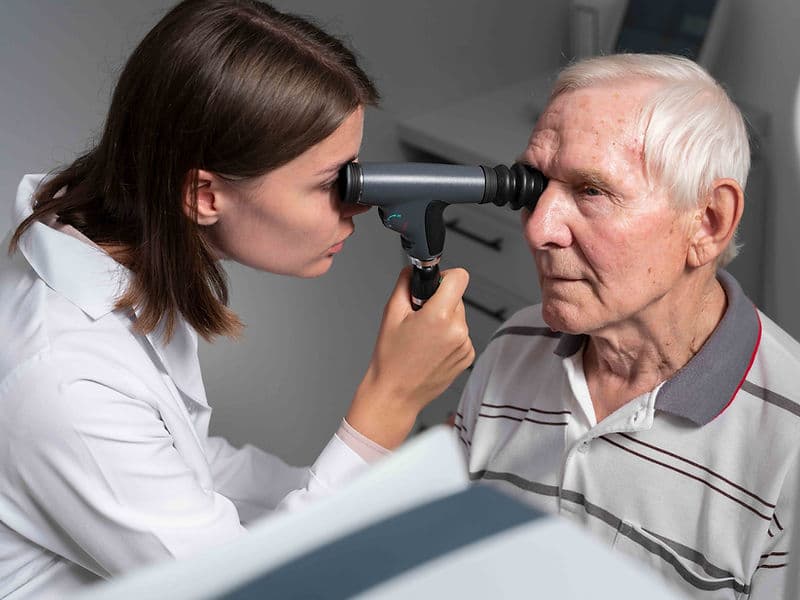
Early Detection Framework: Utilizing OCT and Tonometer technology to identify silent eye diseases years before symptoms appear.
Global Safety Protocols: Strict adherence to international standards for medication schedules and protective care ensures a successful post-operative journey.