Women Care
Obstetrics and Gynecology (OB/GYN) Department
The OB/GYN Department—frequently known as the Center for Women’s Excellence—is a high-activity wing dedicated to the entire spectrum of female reproductive health. This department seamlessly balances the life-affirming experience of childbirth with high-tech surgical interventions for complex conditions like endometriosis and reproductive cancers. For international patients, this wing offers a "Well-Woman" care model, integrating compassionate maternity services with elite "keyhole" surgical expertise.
A Multidisciplinary Circle of Women’s Health Experts
Our department is staffed by a specialized team of clinicians who manage health from adolescence through menopause:
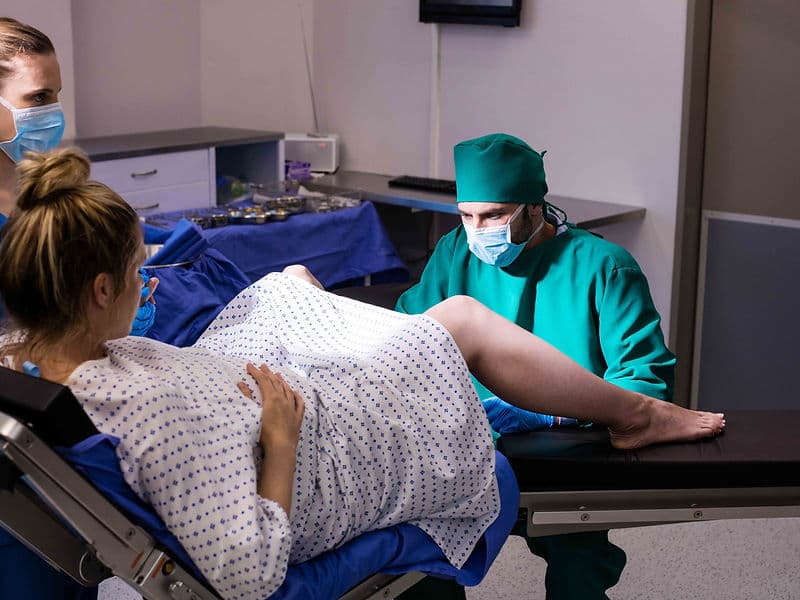
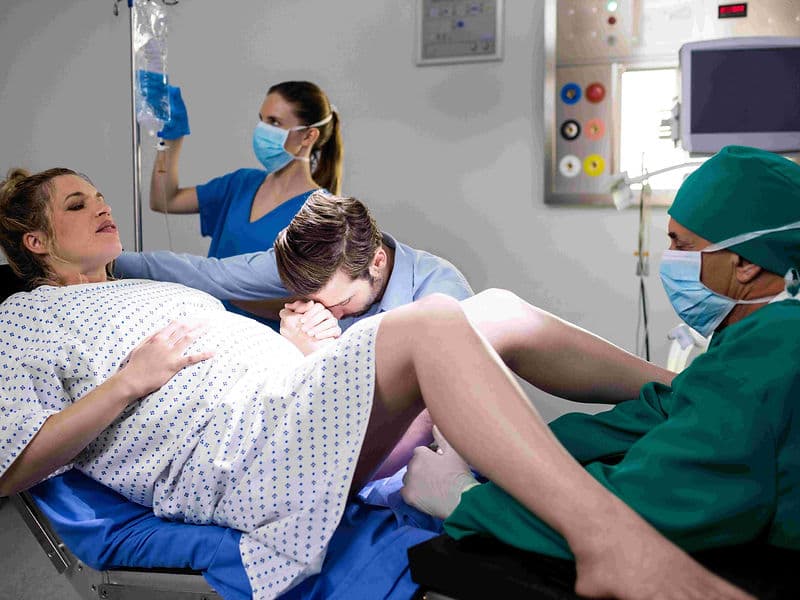
Obstetricians: Primary experts who focus on pregnancy and childbirth, managing everything from natural, painless labor to emergency C-sections.
Gynecologists: Skilled surgeons who treat reproductive organs, managing conditions like PCOS, fibroids, and pelvic pain.
Fetal Medicine Specialists: Highly specialized doctors who treat the baby as a patient while still in the womb, utilizing advanced genetic mapping.
Reproductive Endocrinologists (IVF Specialists): The "fertility architects" who manage In-Vitro Fertilization, egg freezing, and complex hormonal balancing.
Gynaec-Oncologists: Specialized surgeons dedicated to the treatment of cancers affecting the cervix, ovaries, and uterus.
Urogynaecologists: Experts focused on pelvic floor restoration and the treatment of urinary incontinence or organ prolapse.
Advanced Technology and "Incisionless" Care
The department utilizes specialized imaging and miniaturized surgical tools designed specifically for the delicate pelvic cavity:
3D/4D Fetal Ultrasound: High-resolution scanners that provide real-time video of the developing fetus for precise developmental monitoring.
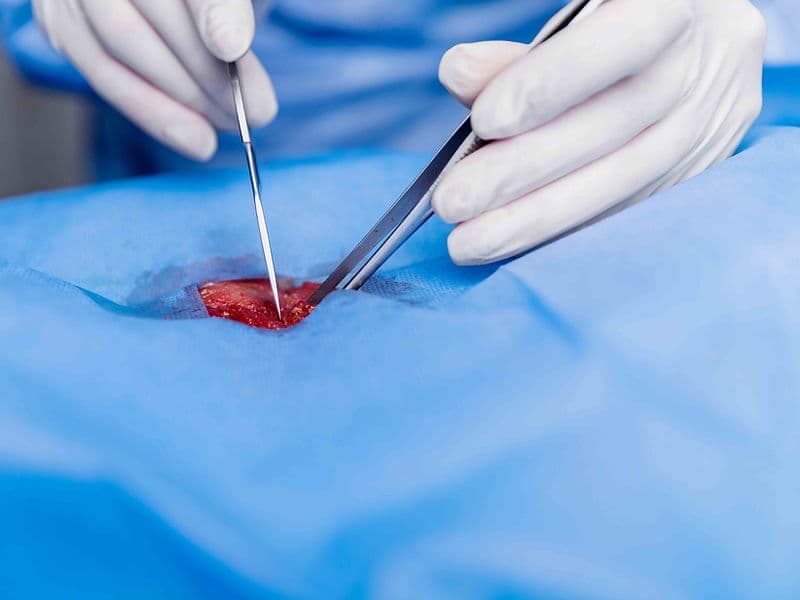
"Single-Port" Laparoscopy: Advanced instruments that allow for major surgeries (like cyst removal) through a single tiny incision in the belly button, leaving almost no visible scar.
Hysteroscope & Colposcope: Miniaturized cameras and microscopes used for incision-free inspections of the uterus and cervix to catch precancerous changes early.
Cardiotocography (CTG) Systems: Vital labor-ward technology that monitors the baby’s heartbeat and mother's contractions simultaneously for 24/7 safety.
Advanced IVF Clean-Rooms: High-security labs where embryos are created and genetically screened (PGT) to increase the success rate of healthy pregnancies.
Specialized Functional and Diagnostic Areas
To support the journey from wellness to motherhood, the department integrates specialized recovery and diagnostic zones:
Modern LDR Suites: All-in-one Labour, Delivery, and Recovery rooms designed for a home-like feel while housing "hidden" state-of-the-art medical support.
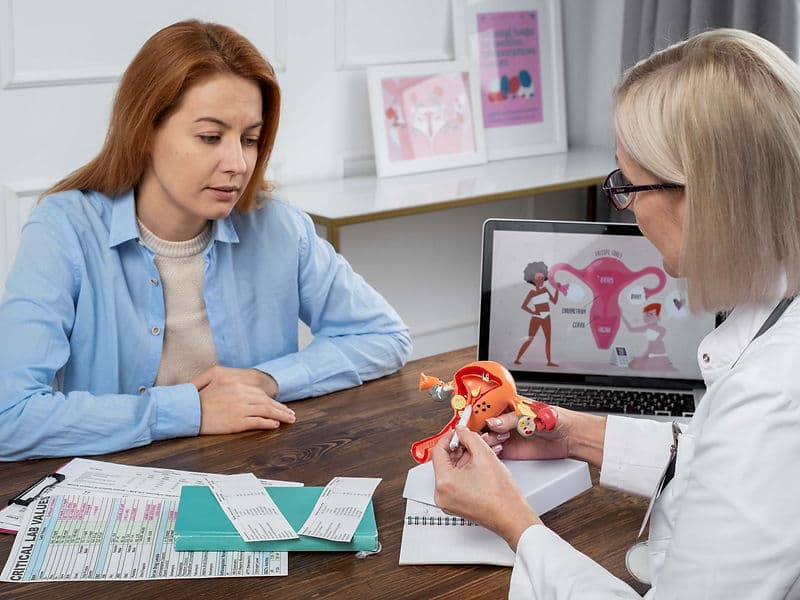
The Well-Woman Clinic: A dedicated outpatient hub for routine screenings, including Pap smears, mammography, and menopause counseling.
Maternal Intensive Care (MICU): A high-intensity monitoring unit specifically for mothers facing complex complications like extreme high blood pressure.
Fetal Diagnostic Center: A specialized area for "Level-II" ultrasounds and amniocentesis to ensure the highest standards of prenatal health.
International Family Suite: A private sanctuary for global families to coordinate travel logistics, maternity packages, and pediatric transitions.
A Focus on Safety and Empowered Care
The modern OB/GYN experience is designed to be as minimally invasive and comfortable as possible:
Painless Labour Protocols: 24/7 access to specialized epidural services ensures a controlled and comfortable delivery process.
Nerve-Sparing Surgery: Utilizing high-definition scopes to remove fibroids or treat endometriosis while preserving reproductive function.
Integrated Screening: Combining annual Pap smears with HPV testing to ensure cervical health is monitored with global accuracy standards.
Holistic Postpartum Support: Dedicated care pathways for the "Fourth Trimester," focusing on physical healing, lactation support, and pelvic floor rehabilitation.